You might not realize how hard your jaw is working until the damage is already underway. Morning headaches that start at the temples. A dull ache that radiates from the jaw into the ear. Teeth that feel sore for no clear reason. A clicking sound every time you open your mouth wide enough to yawn.
These are signs of temporomandibular joint dysfunction and chronic jaw clenching, conditions that affect millions of people yet often go undiagnosed for years. Patients try night guards, adjust their diet, and manage flare-ups with ibuprofen. Some find partial relief. Many do not.
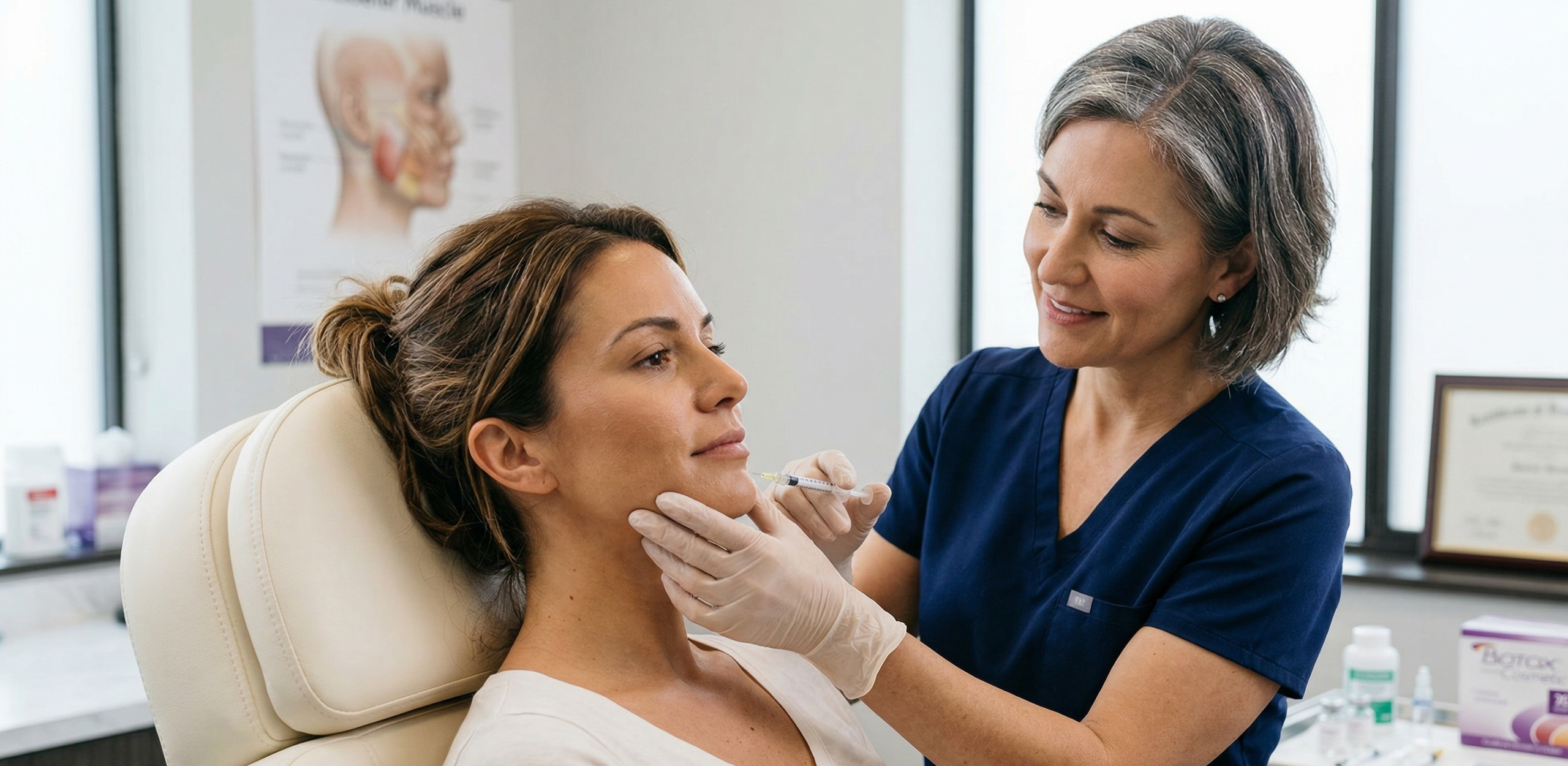
Botox has changed the equation. Originally known for its cosmetic applications in smoothing fine lines and wrinkles, neurotoxin therapy has become one of the most effective non-surgical tools for managing TMJ-related pain and involuntary jaw clenching. At iBeauty Medical in Sylvania, Ohio and Bloomfield Hills, Michigan, we use targeted Botox injections to relax overactive jaw muscles, reduce grinding force, and give patients the relief they have been searching for.
What TMJ dysfunction actually is
The temporomandibular joint sits on each side of your head, just in front of the ears. It connects the lower jaw to the skull and allows you to chew, speak, yawn, and swallow. When this joint or the muscles surrounding it become strained, inflamed, or overworked, the resulting condition is called temporomandibular joint dysfunction, commonly shortened to TMJ or TMD.
TMJ dysfunction is not a single diagnosis. It is an umbrella term that covers joint inflammation, disc displacement, and myofascial pain in the muscles that control jaw movement. The most common culprit behind chronic jaw pain is muscular: the masseter and temporalis muscles become hypertonic, meaning they contract with excessive force and fail to fully relax.
Bruxism, the medical term for habitual teeth grinding or clenching, is the primary driver of this muscular overload. It comes in two forms. Awake bruxism involves clenching during the day, often triggered by stress, focus, or anxiety. Many people do this without awareness, pressing their teeth together while working, driving, or scrolling through their phone. Sleep bruxism happens at night and tends to generate even more force because there is no conscious control to moderate the intensity.
Over time, the muscles grow larger and stronger from constant engagement. The masseter, already one of the most powerful muscles in the body relative to its size, can develop visible bulk along the jawline. The result is a self-reinforcing cycle: the stronger the muscle becomes, the more force it generates, and the worse the symptoms get.
How you know it is more than stress
Many patients dismiss early TMJ symptoms as stress-related tension. And while stress does contribute to clenching, TMJ dysfunction produces specific patterns that set it apart from ordinary tension.
Common signs of TMJ dysfunction and chronic clenching:
Pain or soreness in the jaw upon waking, especially near the ears. Frequent tension headaches concentrated at the temples. Teeth that appear worn, chipped, or flattened. A clicking or popping sound when opening or closing the mouth. Difficulty opening the mouth fully. Facial fatigue after meals or long conversations. Neck and shoulder tightness that seems connected to jaw tension.
If several of these sound familiar, the issue likely extends beyond everyday stress. A provider experienced in facial anatomy can evaluate whether Botox is a suitable next step.
Why Botox works for TMJ
Botox, or onabotulinumtoxinA, is a purified neurotoxin that temporarily blocks the chemical signal between a nerve and a muscle. When injected into an overactive muscle, it reduces the muscle’s ability to contract with full force. The muscle does not shut off entirely. It simply relaxes enough to break the cycle of hyperactivity.
For TMJ patients, this mechanism is exactly what is needed. The masseter muscle, which runs along the angle of the jaw, is the primary target. In chronic clenchers and grinders, this muscle is often visibly enlarged and palpably tight. Botox reduces the intensity of its contractions so the joint is no longer absorbing excessive force during sleep and throughout the day.
The temporalis muscle, which spans the side of the head from the temple to the jaw, may also be treated depending on the patient’s symptoms and anatomy. When both muscles are addressed, patients often report a significant reduction in headaches as well as jaw pain.
This is the same neurotoxin used in cosmetic treatments for expression lines, and it is the same product used therapeutically for chronic migraines. The difference is where it is placed and the clinical goal behind the injection.
The appointment itself
One of the most common questions patients ask is what the actual treatment feels like. The answer is straightforward: it is quick, it is tolerable, and it requires no preparation or downtime.
Before treatment
Your provider will assess your jaw by palpating the masseter and temporalis muscles. You may be asked to clench so the provider can feel the muscle bulk and locate the areas of greatest tension. This hands-on evaluation determines exactly where the injections should go and how many units are appropriate.
There is no need to stop eating or drinking before the appointment. Patients who want to minimize bruising may choose to avoid blood-thinning supplements like fish oil, vitamin E, and aspirin for a few days beforehand, though this is optional.
During treatment
The injections themselves take roughly 10 to 15 minutes. A fine needle delivers small amounts of Botox into multiple points within each masseter muscle. Some providers also treat the temporalis. Most patients describe the sensation as a brief pinch at each injection site.
No anesthesia is required. The needles used are extremely small, and the discomfort is minimal. You can return to work, eat normally, and resume all regular activities immediately after leaving the office.
After treatment
There is no visible downtime. Some patients notice mild tenderness at the injection sites for a day, similar to the feeling after a blood draw. Bruising is rare but possible. Ice can be applied if needed.
The Botox begins to take effect within a few days. Most patients feel noticeable improvement in jaw tension and pain within one to two weeks. Full effect is typically reached around the four-week mark.

What results look like
Patients who receive Botox for TMJ and clenching consistently describe a sense of physical release they did not know was possible. The jaw feels lighter. Morning headaches diminish or disappear. Teeth no longer feel sore. The constant low-grade ache that had become background noise simply quiets.
Beyond pain relief, there is often a visible change. Chronic clenchers frequently develop a squared or widened jawline from masseter hypertrophy. As Botox relaxes the muscle over several weeks, the muscle gradually reduces in size. The lower face appears slimmer and more contoured, a welcome cosmetic benefit that many patients did not anticipate.
Results typically last three to four months. With consistent treatment, many patients find that the intervals between appointments gradually increase as the muscle retrains and the clenching habit weakens over time.
It is also common for patients to sleep better. When the jaw is not generating high levels of force throughout the night, sleep quality improves. Patients who previously woke multiple times with jaw tension or headaches often report sleeping through the night within a few weeks of treatment.
Treatment timeline at a glance
Timeframe | What to expect |
Day 1 | Mild tenderness at injection sites. Resume all normal activities immediately. |
Days 3 to 5 | Botox begins to take effect. Some patients notice early softening of jaw tension. |
Weeks 1 to 2 | Noticeable reduction in clenching force, headaches, and jaw soreness. |
Week 4 | Full effect reached. Maximum pain relief and visible slimming of the jawline. |
Months 3 to 4 | Effects gradually wear off. Schedule a maintenance appointment to sustain results. |
Who is a good candidate
Botox for TMJ works best for patients whose pain originates from muscular tension rather than structural damage to the joint itself. If your primary symptoms are jaw soreness, clenching, grinding, tension headaches, and masseter tightness, you are likely a strong candidate.
Patients who have tried night guards or oral splints without sufficient relief often find Botox to be the next logical step. It is also appropriate for patients who wake with jaw pain despite wearing a guard, because the guard protects the teeth but does not reduce the muscular force behind the clenching.
Botox is not the ideal solution for TMJ symptoms caused by disc displacement, joint degeneration, or structural abnormalities within the joint itself. These conditions involve the joint mechanics rather than the surrounding muscles and may require a different treatment path. A thorough assessment during consultation will clarify which category your symptoms fall into.
How many units and which muscles
Dosing for TMJ Botox varies based on the size and strength of the muscles being treated. The masseter is the primary target in nearly all cases. For most patients, each masseter receives 20 to 40 units, distributed across multiple injection points within the muscle.
If the temporalis muscle is also contributing to pain and headaches, an additional 10 to 25 units per side may be placed there. The total dose depends on the severity of symptoms, muscle bulk, and your provider’s clinical judgment.
Precision matters more than volume. Placing the right amount in the right location produces better outcomes than simply using more product. This is why TMJ Botox should be performed by a provider with deep knowledge of facial anatomy and experience treating functional concerns, not just cosmetic ones.
Botox versus a night guard
Night guards and Botox are not competing treatments. They address different parts of the same problem, and for many patients, the best results come from using both.
A night guard creates a physical barrier between the upper and lower teeth. It prevents direct tooth-on-tooth contact and distributes grinding forces more evenly. What it does not do is reduce the force of the clench itself. Patients who grind aggressively can still generate enough muscular pressure to cause jaw pain, headaches, and joint strain even with a guard in place.
Botox addresses the force. By relaxing the masseter, it lowers the intensity of the involuntary contractions that drive clenching and grinding. Together, the guard protects the teeth while the Botox protects the muscles and joint. For patients who have worn a guard faithfully for years and still wake up with soreness, adding Botox often provides the missing piece of the puzzle.
The aesthetic bonus
Many patients come in for TMJ relief and leave with an unexpected cosmetic benefit. When the masseter muscle is chronically overworked, it thickens and widens, much like any muscle that is exercised heavily. This creates a square or heavy appearance along the lower jaw that can make the face look wider than its natural proportions.
As Botox relaxes the masseter over several weeks, the muscle gradually atrophies. The jawline softens and narrows, restoring a more balanced facial shape. For patients who also want to refine the lower face further, this treatment pairs well with dermal fillers along the chin or jawline for added definition and contour.
This dual benefit, functional relief paired with facial refinement, is one of the reasons TMJ Botox has become so popular among patients who might never have considered Botox for purely cosmetic reasons.
What the research supports
Botox for TMJ is not a trend or a workaround. It is backed by a growing body of clinical evidence. Randomized controlled trials have demonstrated that Botox injections reduce pain levels and improve mouth opening in patients with myofascial TMD. Studies involving injections into the masseter have shown measurable decreases in nighttime grinding activity, with symptom improvement lasting approximately three months before retreatment is needed.
Research also supports the safety profile of this application. Side effects are uncommon and typically limited to temporary tenderness or mild bruising at the injection site. When performed by a qualified provider who understands facial anatomy and appropriate dosing, the treatment carries minimal risk.
It is worth noting that Botox for TMJ is considered an off-label use, meaning the FDA has not specifically approved it for this indication. However, off-label use of Botox is well established across many medical specialties, and the evidence supporting its use for jaw clenching and TMJ pain continues to grow. Many orofacial pain specialists and experienced aesthetic providers now consider it a standard part of their treatment toolkit for patients with chronic muscular TMJ symptoms.
What Botox cannot fix
Transparency matters when setting expectations. While Botox is highly effective for muscular TMJ symptoms, it is not a solution for every type of jaw problem.
Structural joint issues. Disc displacement, joint degeneration, or arthritis within the TMJ itself require evaluation by an oral surgeon or TMJ specialist. Botox relaxes muscles but does not repair joint structures.
Inflammatory conditions. If the joint is actively inflamed due to autoimmune disease or acute injury, Botox will not address the underlying inflammation. Anti-inflammatory medications or other interventions may be more appropriate.
An accurate diagnosis before treatment is essential. The goal is not to use Botox indiscriminately but to match it to the right clinical picture. During your consultation, your provider will evaluate the source of your pain and explain whether Botox, a different treatment, or a combination approach is most appropriate for your specific situation.
Building a complete approach
TMJ management often benefits from a layered strategy. Botox addresses the muscular component, but complementary treatments can enhance and extend the results.
Morpheus8 and Forma can improve skin tightness along the jawline and lower face, amplifying the aesthetic benefits of masseter reduction. For patients dealing with stress-related tension throughout the face and neck, infrared light therapy offers a soothing, non-invasive way to support muscle recovery and relaxation between Botox appointments.
Patients managing broader wellness goals may also benefit from IV therapy or booster shots to support overall recovery and stress resilience. At iBeauty Medical, we look at the full picture rather than treating any single concern in isolation.
Frequently asked questions
Is Botox for TMJ painful?
Most patients describe the injections as a brief pinch. The needles are very fine and the treatment takes only 10 to 15 minutes. No anesthesia is needed, and most patients tolerate the procedure comfortably.
How long does it take to feel relief?
Some patients notice early improvement within a few days. Most experience significant relief within one to two weeks. Full results, including visible jawline slimming, are typically reached by four weeks.
Will Botox affect my ability to chew?
No. The goal is to reduce excessive clenching force, not to eliminate normal muscle function. Patients retain full ability to chew, speak, and move their jaw normally. Some patients notice that biting into very hard foods feels slightly different during the first week, but this adjusts quickly.
How often do I need treatment?
Most patients return every three to four months initially. Over time, as the clenching pattern weakens and the muscle becomes less hypertonic, some patients can extend their treatment intervals to every five or six months.
Can I get TMJ Botox and cosmetic Botox at the same appointment?
Yes. Many patients combine TMJ treatment with cosmetic neurotoxin injections for expression lines during the same visit. Your provider will plan the dosing for both areas together.
Is TMJ Botox covered by insurance?
In most cases, cosmetic and therapeutic Botox administered at a med spa is not covered by insurance. However, the investment in consistent treatment often replaces years of spending on guards, pain medications, and dental repairs caused by grinding.
Final Thoughts
Living with chronic jaw pain is exhausting. It wears on your sleep, your concentration, your comfort in your own body. If you have tried managing TMJ symptoms on your own and the relief has been incomplete, Botox may be the intervention that finally changes the pattern.
At iBeauty Medical, we approach TMJ Botox with the same precision and care that defines every treatment we offer. We assess your anatomy, listen to your symptoms, and build a plan that targets the root cause of your discomfort. The goal is not just temporary relief but a lasting shift toward comfort and balance.
If you are ready to explore if Botox for TMJ is right for you, we invite you to book a consultation. Let us help you stop clenching and start living without the pain.